In a highly physical and psychologically demanding, results-based industry, football players are required to train and compete on a regular basis, whilst conditioning coaches strive to preserve performance, prevent injury and promote physical conditioning. However, how much do we really understand this habitual aspect of our lives and how this essential process is part of our physical and mental recovery.
Sleep. We partake in it for several hours a day, many hours a week and it is thought that if the average human lives till their 79 years of age, 26 of those will be spent sleeping and a further 7 years just trying to get to sleep. But do we really understand why this habitual aspect of our lives is required. For the elite athlete, do we pay sleep the respect it deserves or are we taking this essential process of physical and mental recovery for granted?
Somewhere in the blue light, technological evolution, weekends have been lost to work as hours have increased and the need for social connectivity 24 hours a day is now the norm. On a global scale, the human-race now ingests stimulants to keep us awake, tablets to help switch off and burns the candle at both ends with little consideration as to the effects on the body and mind. Research in recent years has demonstrated links between sleep and diseases such as obesity and diabetes (8) to showing that our brains wash away their waste toxins during sleep (55).
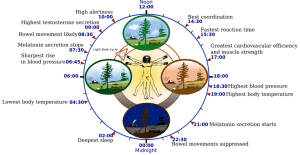
Before prescribing any athlete with a sleep programme, it is worthwhile that they understand circadian rhythm. This is an internal body clock that regulates our internal systems, functions and processes throughout a 24-hour period. Our bodies work in harmony with a daily timing schedule which is shown in the following figure. Circadian rhythm can be affected by both endogenous factors (light, temperature) and exogenous factors (social interaction, meals and exercise).
Sleep stages can be divided into two main types, rapid eye movement (REM) and non-REM (NREM) sleep. NREM sleep is divided into four stages, which progressively develop in the depth of sleep (9). Core body temperature also decreases within these stages, whilst peripheral temperature is increased. The difference in body temperature is most apparent during the first hour of sleep (21). Several studies have investigated the effects of passively changing body temperature prior to sleep. Increasing body temperature by taking a warm shower before bed has been shown to promote thermoregulatory changes, decrease time to initiation of sleep (latency) and improve sleep efficiency (17; 18), including that in youth football players (54). Given the known relationships between sleep and thermoregulation, circadian rhythm and its daily regulation of body temperature is vital to human sleep.
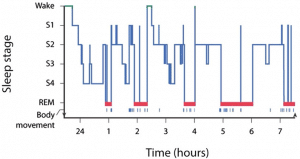
REM sleep is characterised by muscle atonia (loss in muscle tone), bursts of REM and dreaming. It is suggested that deep sleep is most important for optimum anabolic conditions and recovery. Little research is available involving athletes, however, there is evidence in support of this theory, which concludes the release of growth hormone during deep sleep is at its largest within the first hour of sleep (51), placing importance on sleep onset for recovery and growth. The figure below reproduced from Carskadon and Dement (2011) shows how recovery is maximised at varying periods of deep sleep, which interestingly seem to occur roughly every 90 minutes.
Vgontzas et al. (2004) reported that modest chronic sleep loss is associated with significant sleepiness, impairment of psychomotor performance and increased secretion of IL-6 and/or TNFα. IL-6 or Interleukin-6 is an important cytokine, mediating immune and inflammatory responses, whilst also acting as a regulator in metabolic, regenerative and neural processes (43). Tumor necrosis factor (TNFα) is a cell signalling protein (cytokine) involved in early inflammatory events which activate signalling pathways for cell survival, apoptosis and cellular differentiation (20). Of course, an increased secretion of these two cytokines indicates the body’s response to stress.
Another study into sleep loss and inflammatory markers have highlighted increases in C-reactive protein or CRP (28). CRP is the major marker of the formation of plasma proteins in response to an inflammatory stimulus, which is largely controlled by IL-6 and TNFα (10). The chronic release of such markers is supposedly predictive of future cardiovascular morbidity (29), whilst further epidemiologic studies have concluded that CRP is a predictor of both a long and short-term risk of stroke and myocardial infarction in men and women (11; 41).
Sleep has been stated as the major reason for fatigue/tiredness in both healthy adults and athletes (12). A study by Van Dongen et al. (2003) showed that sleep restriction down to 6 hours a night, was associated with a deterioration of psychomotor performance. There is much literature available studying sleep deprivation among athletes, which suggests that sleep and recovery are pivotal to adaptation and subsequent performance (39; 45; 50); associated decreases in competitive performance and reduced levels of determination/intensity in training (40; 4); mood and cognition impairment (5, 49, 22), greater levels of fatigue, depression, and confusion (53), reduced levels of metabolic and weight management (44; 16), and significant impairment of glucose metabolism with severe sleep restriction (47). Ultimately, with the deterioration in mood, there is an impact on athletes participating in training and competition (38). Factors associated with sleep deprivation have included but are not limited to; travelling across time zones, nervous anticipation prior to competition, parenting young children and making physiological composition changes.
Comparatively, in a study by Blumert et al. (2007), they researched weightlifting performance using the snatch, clean & jerk, and front squat; and concluded that lifting performance wasn’t significantly altered after a period of sleep deprivation. Similarly, studies on anaerobic wingate performance have shown no performance decrements (6; 31; 46). There is reasonable evidence to suggest that to witness a significant decrement in performance, a sleep deprivation period of a more substantial duration (beyond 30 hours) needs to occur. Souissi et al. (2003) reported significant decreases in peak and average power generating capacity,
whilst Bulbulian et al. (1996) reported significant decreases in isokinetic performance after 36 and 30 hours respectively. Takeuchi et al. (1985) reported that 64 hours of sleep deprivation resulted in decreased vertical jump performance and isokinetic knee extension strength. Interestingly, Reilly & Piercy (1994) suggested that performance decrements in the more skill-related tasks or the more compound exercises such as the deadlift, leg press, and bench press were greater, while there were no alterations in more isolated exercises such as a bicep curl.
Notable decreases in performance during periods of sleep deprivation are thought to be associated with acute alterations in basal levels of cortisol and testosterone (37). There is varying evidence in relation to basal cortisol levels during periods of sleep deprivation with some studies reporting increases (34; 38), decreases (3), or no change at all (33; 27). On the other hand, it appears that testosterone levels remain depressed during sleep deprivation (1; 32; 33).
Although whilst studying weightlifting performance, Blumert et al. did not find any significant performance decrements after sleep deprivation, it was concluded that measures of vigour, fatigue, confusion, total mood disturbance, and sleepiness were all significantly altered by sleep loss. Pilcher and Huffcutt (1996) also found that psychological performance variables were more notably affected within the earlier phases (<24 hours) of sleep loss. Similar decreases in psychological markers of performance were recorded by Meney et al. (1998), which suggests that individual mood state and physical application are closely associated, with extrinsic motivation being the primary driver for training and competitive performance. Overall, it appears that the greater the amount of total stress (e.g. sleep deprivation, caloric deficit, prolonged work), the more pronounced the changes in
psychological measures associated with mode states. It is possible that psychological markers are visible in advance of physiological performance markers, which may explain how performance in power or strength activities is not significantly altered in the acute phases (<24hours) of sleep loss.
Increasing habitual sleep duration from 7-8 hours per night has been shown to result in faster reaction times and lower levels of daytime sleepiness and fatigue (19). Sargent et al. (2014) reported a marked difference in sleep duration on training days and rest days when athletes were required to train early in the morning. It was found athletes who attempted to advance their bedtime the night before training days, still obtained significantly less time in bed, sleep duration and earlier offset times than nights prior to rest days, suggesting that shorter sleep duration is associated with higher levels of pre-training fatigue. Leeder et al. (2012) reported reduced sleep duration in Olympic athletes during an out of competition training phase, whilst Mah et al. (2011) and Fietze et al. (2009) reported lower than recommended sleep duration in male collegiate basketball players and professional ballet dancers respectively during periods of intense training in relation to their sport.
When designing training schedules, coaches should be aware of the implications of the timing of training sessions on sleep and fatigue and provide countermeasures to be included into the day to support the player. Some considerations may include:
-
- Day-time napping. Waterhouse et al. (2007) concluded that sleep deprived males who took an early afternoon nap for 30 minutes, improved 2m and 20m sprint time, along with pre/post-test heart rate, short term memory, alertness and sleepiness.
- Consume some high GI carbohydrate at least 1hr prior to bedtime, such as white rice, white bread, and potatoes. Porter and Horne (1981) and Afhagi et al. (2007) found that this led to an increase in REM sleep and sleep onset occurred quicker.
- Levels of fat intake should be monitored as Grandner et al. (2010) concluded that this reduced total sleep time.
- Allow for adequate protein intake as this is shown to decrease waking episodes (25).
- Add tart cherry and kiwi fruit into the diet as these contain high levels of melatonin (sleep inducing hormone) which has been shown to improve sleep quality, efficiency and total sleep time (24; 34; 14).
- Diets with restricted total calorific intake may find sleep quality is disturbed (15).
- Foods rich in tryptophan (precursor to melatonin) should be consumed in small doses to help improve both sleep latency and sleep quality. This can be achieved by consuming approximately 300 g of turkey or approximately 200 g of pumpkin seeds (15).
- According to Carskadon and Dement (2011), maximum recovery periods of sleep occur roughly every 90 minutes (the duration of a football match). It may be to useful to consider how many 90-minute cycles can be achieved throughout a night’s sleep, rather than focusing on the number of hours.
References
- Aakvaag, A., Sand, T., Opstad, PK., and Fonnum, F. 1978. Hormonal changes in serum in young men during prolonged physical strain. Eur. J. Appl. Physiol. 39, 283-291.
- Afhagi et al. 2007. High-glycemic-index carbohydrate meals shorten sleep onset. Am J Clin Nutr, 85(2), 426-430.
- Akerstedt, T., Palmblad, J., De La Torre, B., Marana, R., and Gillberg, M. 1980. Adrenocortical and gonadal steroids during sleep deprivation. Sleep 3, 23-30.
- Atkinson, G., Reilly, T., Waterhouse, J., and Winterburn, S. 1997. Pharmacology and the travelling athlete. In: The Clinical Pharmacology of Sport and Exercise. T. Reilly and M. Orme, Eds. Amsterdam: Elsevier Science, 293-301.
- Belenky, G., et al. 2003. Patterns of performance degradation and restoration during sleep restriction and subsequent recovery: a sleep dose–response study. J Sleep Res. 12(1), 1-12.
- Bryant, WK., Hill, DW., and Smith, JC. 1991. Sleep deprivation: No effect on anaerobic power and capacity. Med. Sci. Sports Exerc. 23, S11.
- Bulbulian, R., Heaney, JH., Leake, CN., Sucec, AA., and Sjoholm, NT. 1996. The effect of sleep deprivation and exercise load on isokinetic leg strength and endurance. Eur. J. Appl. Physiol. 73, 273-277.
- Buxton, OM., Cain, SW., O’Connor, SP., Porter, JH., Duffy, JF., Wang, W., Czeisler, CA., Shea, SA. 2012. Adverse metabolic consequences in humans of prolonged sleep restriction combined with circadian disruption. Science Translational Medicine.
- Carskadon MA., Dement WC. 2011. Normal human sleep: an overview. In: Kryger MH, Roth T, Dement WC, editors. Principles and practice of sleep medicine. 5th ed. St. Louis: Elsevier, 16-26.
- Castell, JV., Gomez-Lechion, MJ., David, M., et al. 1990. Acute phase response of human hepatocytes: regulation of acute-phase protein synthesis by interleukin-6. Hepatology 12, 1179-1186.
- Danesh, J., Whincup, P., Walker, M., et al. 2000. Low grade inflammation and coronary heart disease: prospective study and updated meta-analyses. BMJ, 321, 199-204.
- Fallon, KE. 2007. Blood tests in tired elite athletes: expectations of athletes, coaches and sport science/sports medicine staff. Br J Sports Med, 41(1), 41-44.
- Fietze, I., Strauch, J., Holzhausen, M., et al. 2009. Sleep quality in professional ballet dancers. Chronobiol Int. 26, 1249-1262.
- Garrido, M., et al. 2010. Valley cherry-enriched diets improve nocturnal rest and increase 6-sulfatoxymelatonin and total antioxidant capacity in the urine of middle-aged and elderly humans. J Gerontol A Biol Sci Med Sci, 65, 909-914.
- Halson, SL. 2014. Sleep in elite athletes and nutritional interventions to enhance sleep. Sports Medicine, 44(1), 13-23.
- Hogenkamp, PS., et al. 2013. Acute sleep deprivation increases portion size and affects food choice in young men. Psychoneuroendocrinology: 38, 1668-1674.
- Horne, JA., Shackell, BS. 1987. Slow-wave sleep elevations after body heating-proximity to sleep and effects of aspirin. Sleep, 10, 383-392.
- Jordan, J., Montgomery, I., and Trinder, J. 1990. The effect of afternoon body heating on body temperature and slow wave sleep. Psychophysiology, 27, 560-566.
- Kamdar, BB., Kaplan, KA., Kezirian, EJ., and Dement, WC. 2004. The impact of extended sleep on daytime alertness, vigilance, and mood. Sleep Med, 5, 441-448.
- Kawasaki, H., et al. 2002. Identification of genes that function in the TNFα-mediated apoptotic pathway using randomized hybrid ribozyme libraries. Nat Biotechnol, 20, 376-80.
- Krauchi, K., Wirz-Justice, A. 2001. Circadian clues to sleep onset mechanisms. Neuropsychopharmacology, 25, S92-S96.
- Lastella, M., et al. 2015. Sleep/wake behaviour of endurance cyclists before and during competition. J Sports Sci, 33(3), 293-299.
- Leeder, J., Glaister, M., Pizzoferro, K., et al. 2012. Sleep duration and quality in elite athletes measured using wristwatch actigraphy. J Sports Sci, 30, 541-545.
- Lin, HH., et al. 2011. Effect of kiwifruit consumption on sleep quality in adults with sleep problems. Asia Pac J Clin Nutr, 20, 169-174.
- Lindseth, G. et al. et al. 2013. Nutritional effects on sleep. West J Nurs Res., 35, 497-513.
- Mah, CD., Mah, KE., Kezirian, EJ., and Dement, WC. 2011. The effects of sleep extension on the athletic performance of collegiate basketball players. Sleep, 34, 943-950.
- Martin, BJ., Bender, PR., and Chen, H. 1986. Stress hormonal response to exercise after sleep loss. Eur. J. Appl. Physiol, 55, 210-214.
- Meier-Ewert, HK., et al. 2004. Effect of Sleep Loss on C-Reactive Protein, an Inflammatory Marker of Cardiovascular Risk. Journal of the American College of Cardiology, 43(4), 678-683.
- Meney, I., Waterhouse, J., Atkinson, G., Reilly, T., and Davenne, D. 1998. The effect of one night’s sleep deprivation on temperature, mood, and physical performance in subjects with different amounts of habitual physical activity. Chronobiol. Int, 15, 349-363.
- Mougin, F., Bourdin, H., Simon-Rigaud, ML., Didier, JM., Toubin, G. and Kantelip, JP. 1996. Effects of a selective sleep deprivation on subsequent anaerobic performance. Int. J. Sports Med, 17, 115-119.
- Opstad, P.K., and Aakvaag, A. 1982. Decreased serum levels of oestradiol, testosterone and prolactin during prolonged physical strain and sleep deprivation, and the influence of a high calorie diet. Eur. J. Appl. Physiol, 49, 343-348.
- Opstad, P.K., and Aakvaag, A. 1983. The effect of sleep deprivation on the plasma levels of hormones during prolonged physical strain and calorie deficiency. Eur. J. Appl. Physiol, 51, 97-107.
- Opstad, P.K., Aakvaag, A., and Rognum, TO. 1980. Altered hormonal response to short-term bicycle exercise in young men after prolonged physical strain, caloric deficit, and sleep deprivation. Eur. J. Appl. Physiol, 45, 51-62.
- Pigeon, WR., et al. 2010. Effects of a tart cherry juice beverage on the sleep of older adults with insomnia: a pilot study. J Med Food, 13, 579-583.
- Pilcher, J.J., and Huffcutt, AI. 1996. Effects of sleep deprivation on performance: A meta-analysis. Sleep, 19, 318-326.
- Porter, JM., and Horne, JA. 1981. Bed-time food supplements and sleep: effects of different carbohydrate levels. Electroencephalogr Clin Neurophysiol, 51(4), 426-433.
- Radomski, M.W., Hart, LE., Goodman, JM., and Plyley, MJ. 1992. Aerobic fitness and hormonal responses to prolonged sleep deprivation and sustained mental work. Aviat. Space Environ. Med, 63, 101-106.
- Reilly, T., Atkinson, G., and Waterhouse, J. 1997. Biological Rhythms and Exercise. Oxford, England: Oxford University Press.
- Reilly, T., and Deykin, T. 1983. Effects of partial sleep loss on subjective states, psychomotor and physical performance tests. J. of Hum. Move. Stud, 9, 157-170.
- Reilly, T., and Piercy, M. 1994. The effect of partial sleep deprivation on weight-lifting performance. Ergonomics, 37, 107-115.
- Ridker, PM. 2001. High-sensitivity C-reactive protein: potential adjunct for global risk assessment in the primary prevention of cardiovascular disease. Circulation, 103, 1813-1818.
- Sargent, C., Lastella, M., Halson, SL., Roach, GD. 2014. The impact of training schedules on the sleep and fatigue of elite athletes. Chronobiology International, 31(10), 1160-1168.
- Scheller, J., Athena, C., Schmidt-Arras, D., Rose-John, S. 2011. The pro- and anti-inflammatory properties of the cytokine interleukin-6. Biochimica et Biophysica Acta (BBA) – Molecular Cell Research, 1813(5), 878-888.
- Schmid, SM., et al. 2011. Disturbed glucoregulatory response to food intake after moderate sleep restriction. Sleep, 34, 371-377.
- Shephard, RJ. 1984. Sleep, biorhythms and human performance. Sports Med, 1, 12-27.
- Souissi, N., Sesboue, B., Gauthier, A., Larue, J., and Davenne, D. 2003. Effects of one night’s sleep deprivation on anaerobic performance the following day. Eur. J. Appl. Physiol, 89, 359-366.
- Spiegel, K., Leproult, R., Van Cauter, E. 1999. Impact of sleep debt on metabolic and endocrine function. Lancet, 354, 1435-1439.
- Takeuchi, L., Davis, GM., Plyley, M., Goode, R., and Shephard, RJ. 1985. Sleep deprivation, chronic exercise and muscular performance. Ergonomics, 28, 591-601.
- Torabi Nami, M., and Sadeghniaat, K. 2011. Understanding the interplay between neurobiochemistry of sleep–wake systems and cognition. Webmed Central Brain, 2(10), 1-10.
- Vanhelder, T., and Radomski, MW. 1989. Sleep deprivation and the effect on exercise performance. Sports Med, 7, 235-247.
- Van Cauter, E., Plat, L. 1996. Physiology of growth hormone secretion during sleep. J Pediatr, 128(5), S32-S37.
- Van Dongen, HP., Maislin, G., Mullington, JM., Dinges, DF. 2003. The cumulative cost of additional wakefulness: dose-response effects on neurobehavioral functions and sleep physiology from chronic sleep restriction and total sleep deprivation. Sleep, 2, 117-126.
- Webb, W.B., and Agnew Jr, HW. 1973. Effects on performance of high and low energy-expenditure during sleep deprivation. Percept. Mot. Skills, 37, 511-514.
- Whitworth-Turner, C., Di Michele, R., Muir, I., et al. 2017. A comparison of sleep patterns in youth soccer players and non-athletes. Sci Med Football, 2(1), 3-8.
- Xie, L., Kang, H., Xu, Q., et al. 2013. Sleep drives metabolite clearance from the adult brain. Science, 342(6156), 373-377.